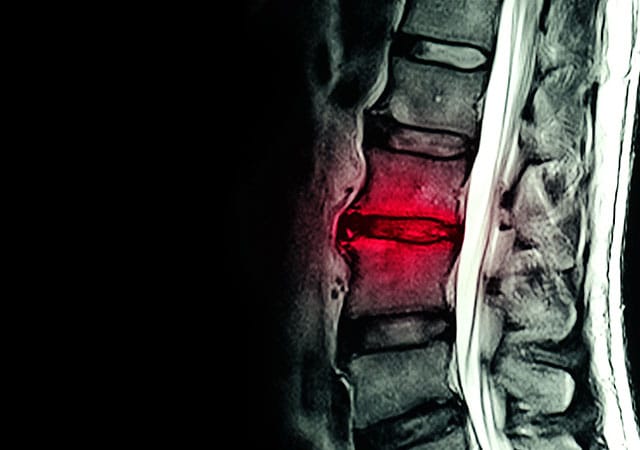
WHAT IS DEGENERATIVE DISC DISEASE?
Our spinal discs serve a crucial role in the body because they absorb the many shocks and compressive forces that our bodies are subjected to. As we age, our spinal discs gradually lose their water and protein content, resulting in the decline of their flexibility, elasticity, and shock-absorbing characteristics. This gradual loss of fluid and function is part of the natural process of growing older and is referred to as Degenerative Disc Disease (DDD).
Degenerative Disc Disease isn’t truly a disease because everyone develops degenerated discs as they age. When the discs leak, people often experience pain and numbness. If there are no leaks, there are no symptoms.
Every degenerated disc begins with an annular tear. The tear progressively worsens to become multiple disc tears, and then finally escalates into disc degeneration. Virtually all MRI and CT studies find that everyone over the age of 60 has some disc degeneration. According to Dr. Pauza, “it is not a disease in the strictest sense of the word, because it occurs in almost everyone.”
WHAT ARE THE SYMPTOMS OF DEGENERATIVE DISC DISEASE?
The symptoms of degenerative disc disease are concentrated in the lower back and neck, but can occur anywhere there is degeneration. They include:
- Mild to severe pain
- Pain that radiates to the buttocks and thighs, as well as the arms and hands
- Pain that is worse when sitting, bending, lifting or twisting
- Pain that is better when changing positions frequently
- Periods of varying pain, from a few days to a few months
- Numbness in the extremities
- Weakness in leg muscles or feet
- Muscle spasms or tension
- A feeling that your neck or back cannot support, loss of balance
WHAT ARE THE RISKS ASSOCIATED WITH DEGENERATIVE DISC DISEASE?
Disc degeneration can lead to bone spurs and to spinal arthritis as discs continue collapsing. Disc degeneration can also lead to other spinal problems such as:
- Spinal stenosis – leads to nerve or spinal cord pinching
- Osteoarthritis in the spine – changes in the joints of the spine due to degeneration
- Spondylolisthesis – where a vertebra slips forward on another vertebra
- Scoliosis – where discs degenerate in lopsided ways causing a curve in the spine
ORDINARY TREATMENTS FOR DEGENERATIVE DISC DISEASE
All standard treatments for degenerative discs consist of some measure of exercise or physical therapy in order to increase the strength and flexibility of the muscles around the spine. This increases the already stifled blood flow to the spine as well. Other treatments are:
- Medication (anti-inflammatory, pain relievers, steroid injections)
- Spinal fusion
- Artificial disc replacement
- Heat and cold therapy
- Spinal mobilization(s)
- TENS (transcutaneous electrical nerve stimulation)
Unfortunately, none of these methods effectively treat the underlying cause of degenerative disc disease, annular tears. Until patients find a solution that actually seals the tears in their discs, they will continue to experience the same painful symptoms that initially led them to seek treatment.
ARE ORTHOBIOLOGICS EFFECTIVE IN TREATING DEGENERATIVE DISC DISEASE?
Even though some pain relief has been seen in a percentage of comprehensive orthobiologic treatments, the need for subsequent injections after the initial treatment is quite common. Receiving multiple injections can be financially costly and frustrating, especially if the treatments do not provide the expected benefits.
Cell-based therapies are unable to effectively treat degenerative discs on their own because these treatments tend to leak out of the discs – they are not properly suited to seal the annular tears that caused the disc to begin to degenerate in the first place. Unfortunately, that leaves patients in the same set of circumstances as patients who seek out more traditional treatment methods.
That is why Dr. Pauza focused on developing a treatment that would be able to treat patients with Degenerative Disc Disease who all suffer from the same underlying issue – annular tears.
WHAT IS FIBRIN?
Fibrin is a crucial molecule that is naturally present within the human body and is involved in the clotting of blood after an injury or trauma. Fibrin is formed when fibrinogen and thrombin combine. Fibrinogen is a glycoprotein that circulates in high concentrations in the blood, and thrombin is an enzyme that works to activate and convert fibrinogen into Fibrin. When an injury occurs, thrombin is released to the specific area that experienced the trauma to initiate the activation of fibrinogen. The Fibrin, together with platelets, forms a hemostatic plug or clot over a wound site.
This naturally occurring combination is able to be replicated outside the body and can be used for surgical purposes. This substance can be separated from the bloodstream and can be activated to produce a glue-like sealant. In the Discseel® Procedure, Fibrin is injected into leaky spinal discs to seal annular tears.
We are even using Fibrin to seal leaky, degenerated discs. The Discseel® Procedure holds great potential to treat this debilitating condition because Fibrin has demonstrated the ability to regrow spinal disc tissue, sufficiently treating annular tears.
CONCLUSION
The success of the Discseel® Procedure can be attributed to the effectiveness of Fibrin. For patients with degenerative disc disease, injecting Fibrin into the spinal discs can achieve positive results.
The Discseel® Procedure is far less invasive, has a much shorter recovery time, and allows patients a greater range of motion than a spinal fusion. The Discseel® Procedure prompts the patient’s body to heal itself without the use of metal hardware and doesn’t have the risk of long-term complications and opioid dependency like spinal fusion.
The Discseel® Procedure carries a high success rate, even for individuals who had previously tried a different spinal procedure but who did not experience favorable results. In fact, 70% of individuals who had undergone previous spinal treatments experienced relief with the Discseel® Procedure.